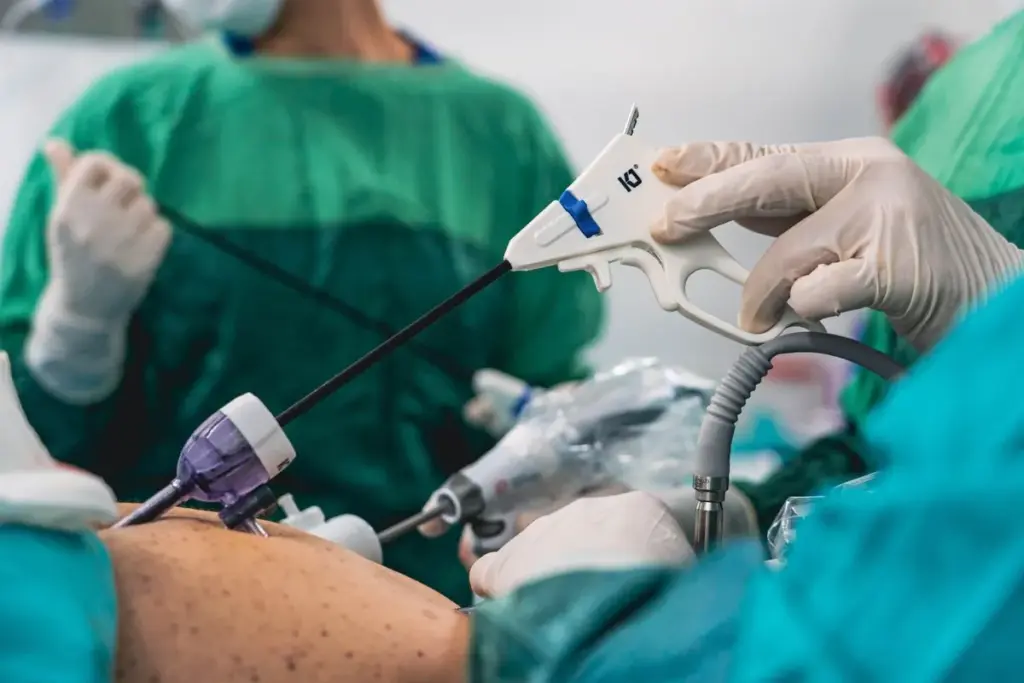
Varicoceles are the most common surgically correctable cause of male infertility, yet a significant number of men who have one either do not know it or have been told it is not worth addressing. The condition involves abnormal enlargement of the veins draining the testicle, similar in concept to varicose veins in the legs, and it affects roughly 15 percent of adult men and 35 to 40 percent of men being evaluated for infertility. At Lazare Urology in Brooklyn, microscopic varicocelectomy is performed for men whose varicocele is affecting fertility, testosterone production, or causing scrotal discomfort. Whether surgery is worth it depends on a set of specific factors that are worth understanding before making that decision.
What a Varicocele Is and Why It Causes Problems
Blood drains from the testicle through a network of small veins called the pampiniform plexus, which converges into the spermatic vein. In a healthy system, one-way valves in these veins prevent blood from flowing backward. When those valves are absent or incompetent, blood pools in the pampiniform plexus rather than draining efficiently upward, causing the veins to dilate and become tortuous. The result is a varicocele.
Varicoceles are graded on a scale of one to three based on size. A grade one varicocele is only detectable with ultrasound or when the patient performs a Valsalva maneuver, a straining action that increases venous pressure. A grade two is palpable without straining. A grade three is visibly enlarged through the scrotal skin. Subclinical varicoceles, detected only on imaging without any physical findings, occupy their own category in the treatment discussion.
The harm varicoceles cause stems primarily from elevated scrotal temperature. The testicles are housed in the scrotum specifically because sperm production requires a temperature two to three degrees Celsius below core body temperature. The pooled, stagnant blood in a varicocele acts as a heat reservoir, warming the testicular environment and impairing the temperature-sensitive processes involved in spermatogenesis. Oxidative stress from the venous congestion also damages sperm DNA and reduces Leydig cell function, the cells responsible for testosterone production.
Left-sided varicoceles are far more common than right-sided ones because of the angle at which the left spermatic vein drains into the left renal vein, creating higher resistance to outflow. Bilateral varicoceles occur in roughly 15 to 20 percent of cases. A right-sided varicocele presenting in isolation, particularly in an older man, warrants evaluation to rule out a retroperitoneal mass compressing the right spermatic vein, as this is an uncommon but clinically significant cause.
How Varicoceles Affect Fertility and Testosterone
The relationship between varicoceles and semen parameters is well established. Men with clinical varicoceles and infertility consistently show lower sperm concentration, reduced motility, and a higher proportion of sperm with abnormal morphology compared to fertile men without varicoceles. These are the three parameters evaluated in a standard semen analysis, and all three tend to improve following successful varicocelectomy.
The improvement is not instantaneous. Spermatogenesis, the process of sperm production, takes approximately 72 days from initiation to mature sperm in the ejaculate. Meaningful changes in semen parameters typically appear in the three-to-six-month range following repair, with some men seeing continued improvement up to 12 months post-operatively. Natural pregnancy rates after varicocelectomy in appropriate candidates are consistently reported in the 30 to 50 percent range over two years, which compares favorably to the cost, complexity, and physical burden of assisted reproduction for couples where the varicocele is the primary identified problem.
The testosterone connection is less universally appreciated. Multiple studies have demonstrated that clinical varicoceles suppress serum testosterone levels, and several have shown meaningful increases in testosterone after repair. The American Urological Association’s guideline on testosterone deficiency now includes varicocelectomy as a consideration for hypogonadal men with a clinical varicocele who prefer to avoid exogenous testosterone and want to attempt to restore natural production. This is a different clinical scenario from the fertility patient, and the decision process differs accordingly.
Who Actually Benefits from Surgery: Separating Signal from Noise
Varicocelectomy is not appropriate for every man with a varicocele, and this is where a lot of the confusion about the procedure’s worth originates. Not every varicocele needs to be fixed. The key questions are whether the varicocele is clinical, meaning detectable on physical examination, and whether there is an objective finding that can be attributed to it.
The American Society for Reproductive Medicine and the AUA both support varicocelectomy when all three of the following conditions are present: the varicocele is palpable on examination, the couple has documented infertility, and at least one semen parameter is abnormal. When these criteria are met, the evidence for benefit is reasonably strong. When they are not, the evidence is weaker and the decision is more nuanced.
Subclinical varicoceles, those found only on ultrasound without physical examination findings, generally do not meet the threshold for surgery based on current evidence. Operating on a varicocele that is not causing a demonstrable physiological effect is unlikely to produce a clinical benefit and exposes the patient to unnecessary surgical risk.
Men with azoospermia, meaning no sperm in the ejaculate, can also benefit from varicocelectomy in select cases. When the azoospermia is non-obstructive and a clinical varicocele is present, repair sometimes results in the return of sperm to the ejaculate, enabling natural conception or at minimum sperm extraction for IVF without requiring a separate surgical retrieval procedure. This is not a guaranteed outcome, but the rates are meaningful enough that varicocelectomy is generally worth attempting before assuming that sperm extraction is the only path.
Microscopic Varicocelectomy: Why Technique Matters
Several surgical approaches exist for varicocelectomy, including open high ligation, laparoscopic repair, and percutaneous embolization. The microsurgical subinguinal approach, performed through a small incision just below the inguinal crease with an operating microscope providing 6 to 25 times magnification, has the best outcomes data of any technique. Recurrence rates after microsurgical varicocelectomy are low, reported at one to two percent in experienced hands compared to 10 to 15 percent for non-microsurgical approaches. Complication rates for hydrocele formation and testicular artery injury are also substantially lower.
The magnification the microscope provides allows the surgeon to identify and ligate the abnormal dilated veins individually while clearly visualizing and sparing the testicular artery and lymphatic vessels. Inadvertent ligation of the testicular artery, which is a real risk in non-magnified approaches, can result in testicular atrophy. Lymphatic vessel damage causes hydrocele, a fluid collection around the testicle, in a significant proportion of non-microsurgical cases. Avoiding both requires the visibility that only the operating microscope provides.
What Recovery Looks Like After Microsurgical Varicocelectomy
Microscopic varicocelectomy is an outpatient procedure performed under general anesthesia and typically takes 30 to 45 minutes per side. Most men return to desk work within two to three days. Physical activity should be restricted for two to three weeks, and heavy lifting and strenuous exercise are avoided for three to four weeks to minimize the risk of hematoma formation and allow the incision to heal soundly.
Scrotal discomfort and swelling in the first week are expected and managed with scrotal support, ice, and over-the-counter anti-inflammatory medication. Sexual activity is typically resumed after two to three weeks. A semen analysis is performed at three and six months post-operatively to assess the response to treatment. For men pursuing fertility, the couple is generally counseled to wait at least three months before concluding that the procedure has reached its full effect on semen parameters.
Getting Evaluated at Lazare Urology in Brooklyn
The varicocele evaluation at Lazare Urology begins with a physical examination, a scrotal ultrasound when indicated, and a semen analysis to establish a baseline. For men whose primary concern is testosterone rather than fertility, serum hormone levels including testosterone, FSH, and LH are assessed to understand the hormonal picture before making a treatment recommendation.
Dr. Jon Lazare performs microscopic varicocelectomy in a certified in-office operating room, combining the precision of the microsurgical technique with the efficiency and personalized attention of a practice designed for exactly this kind of procedure. For men in Brooklyn and across the New York area who have been told they have a varicocele and are wondering whether anything should be done about it, the consultation is where that question gets a direct, evidence-based answer.
Contact Lazare Urology today to schedule an evaluation and find out whether varicocelectomy makes sense for your specific situation and goals.